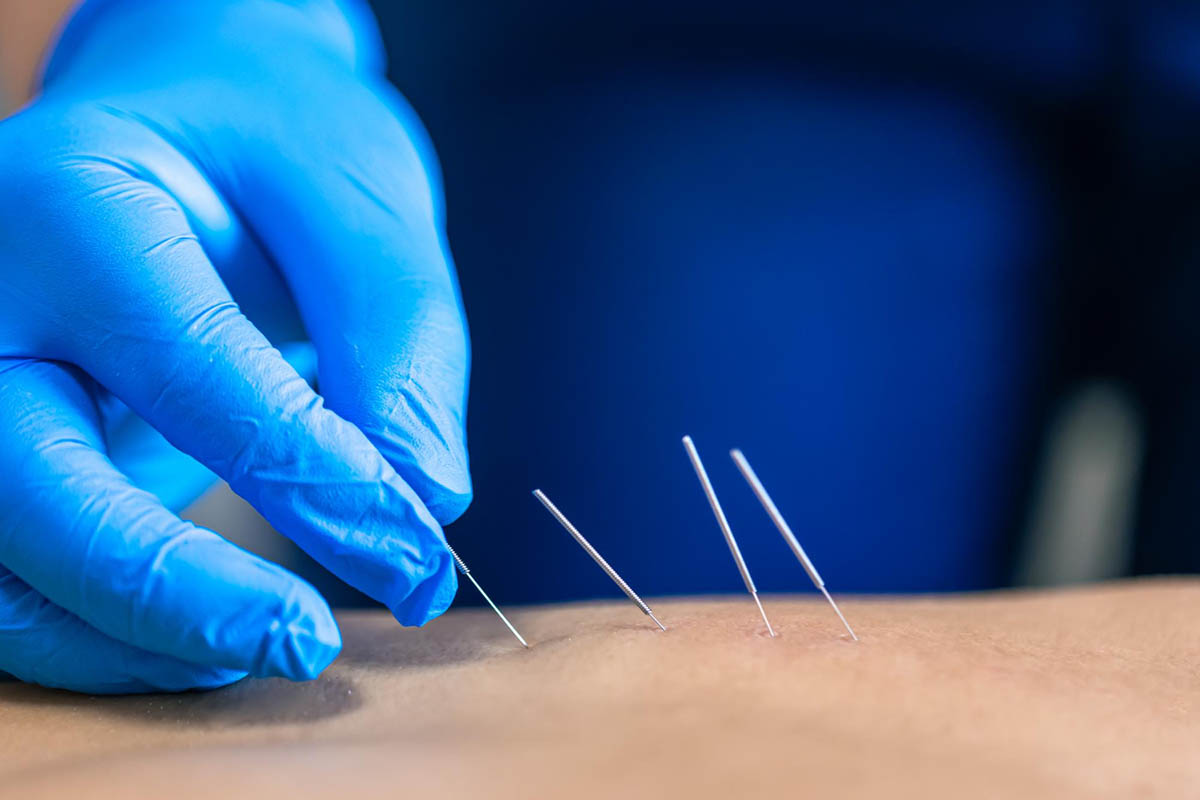
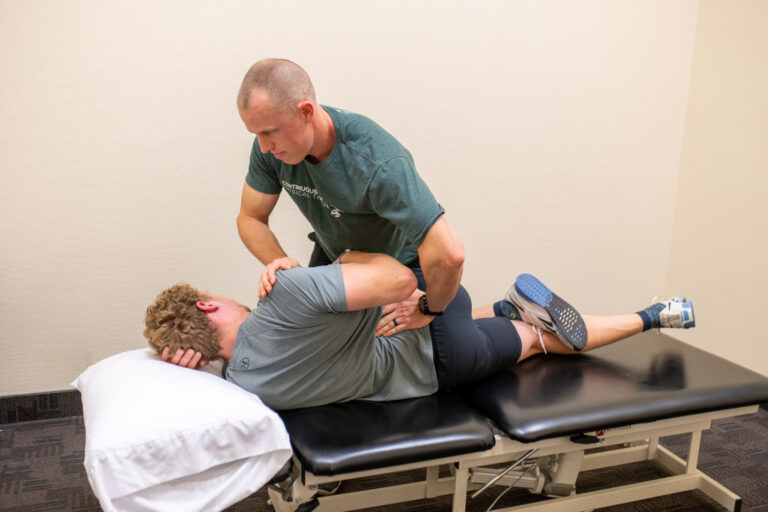
Dry needling has become a popular therapeutic technique for treating musculoskeletal and pelvic issues. In particular, pelvic floor dry needling is being used more often in pelvic floor therapy to address dysfunctions and relieve pain. This technique involves the insertion of thin needles into specific muscle groups or trigger points to relieve pain, increase circulation, and improve muscle function. Pelvic floor dysfunction (PFD) is a common condition, especially among women, and can lead to a variety of symptoms, including pelvic pain, urinary incontinence, and bowel dysfunction. Understanding how dry needling can help with pelvic floor dysfunction can empower patients to manage their symptoms actively.
What is Dry Needling?
Continuous Motion PT offers dry needling for the pelvic floor to treat muscle pain, tightness, and trigger points by inserting thin, sterile needles into the affected areas. Unlike acupuncture, which is rooted in traditional Chinese medicine, dry needling is based on modern Western medicine principles. Dry needling targets muscle knots or “trigger points” to reduce pain, increase flexibility, and improve muscle function.
In pelvic floor therapy, dry needling targets specific muscles within the pelvic region that may contribute to pelvic pain or dysfunction. This technique can help release tightness in the pelvic muscles, improve bladder and bowel control, and relieve discomfort associated with conditions like urinary incontinence, chronic pelvic pain (CPP), and pelvic organ prolapse.
How Dry Needling Helps Pelvic Floor Dysfunction
Pelvic floor dysfunction occurs when the muscles, ligaments, and tissues that support the bladder, uterus, and rectum are weakened, tight, or injured. This dysfunction can result in symptoms such as pain during intercourse, urinary urgency or incontinence, and difficulty with bowel movements. Dry needling for pelvic floor dysfunction can help by targeting the pelvic muscles that contribute to these problems. One in three women will experience a pelvic floor disorder (PFD) in their lifetime. One study reported pain relief, improved mobility, and improved function after 5–7 dry needling sessions in 2 women with CPP. Dry needling can help by targeting the pelvic muscles that contribute to these problems.
Dry needling involves inserting needles into the pelvic floor muscles to help release muscle tension, reduce the formation of trigger points, and improve blood flow to the area. This helps restore the pelvic floor’s normal functioning, essential for proper bladder and bowel control and sexual health. Dry needling also encourages the healing process in muscles that have been overstretched, weakened, or injured.
Benefits of Dry Needling for Pelvic Floor Health
Dry needling offers numerous benefits to those suffering from pelvic floor dysfunction. These benefits include:
Pain Relief
Dry needling is known to provide immediate pain relief. Targeting trigger points in the pelvic muscles can reduce discomfort associated with chronic pelvic pain, bladder discomfort, or painful intercourse. Studies have shown that dry needling can offer significant pain relief after just a few sessions.
Improved Muscle Function
One key benefit of dry needling is that it helps improve muscle function by releasing tightness and increasing flexibility in the pelvic muscles. This can help restore normal movement and function in the pelvic floor, which is crucial for proper bladder, bowel, and sexual health.
Increased Blood Flow
Dry needling can increase blood flow to the treated area, promoting healing and reducing inflammation. Better circulation helps nourish the pelvic muscles and tissues, encouraging them to recover from dysfunction or injury.
Reduction of Trigger Points
Trigger points are tight, painful knots that form in muscles and can cause discomfort and dysfunction. Dry needling targets these trigger points, helping to release them and restore normal muscle function. In the pelvic region, this can lead to a reduction in pain and improvement in overall pelvic floor health.
Improved Bladder and Bowel Control
Dry needling can help improve bladder and bowel control by relaxing the pelvic floor muscles. This can be especially beneficial for individuals suffering from urinary incontinence or constipation, two common issues associated with pelvic floor dysfunction.
Who Can Benefit from Dry Needling for Pelvic Floor Dysfunction?
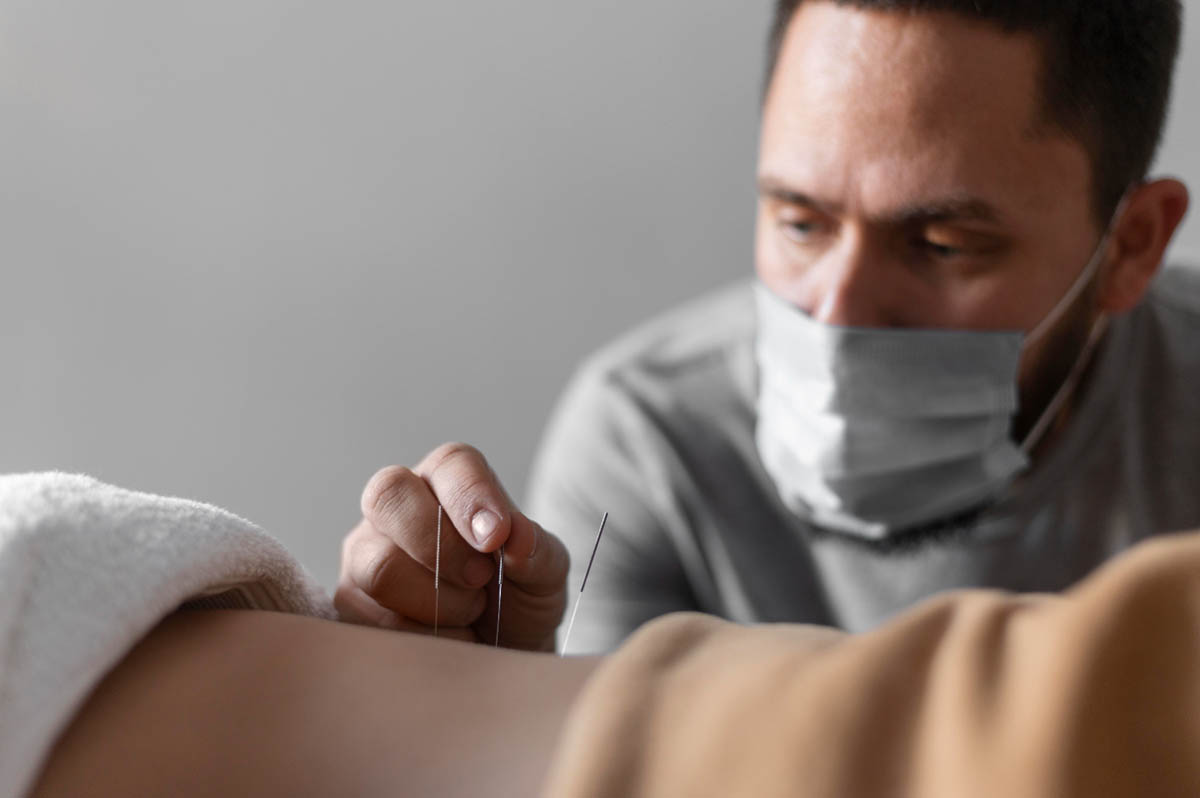
Dry needling for pelvic floor dysfunction can benefit individuals experiencing a variety of symptoms, including:
- Chronic pelvic pain (CPP)
- Urinary incontinence or urgency
- Painful intercourse (dyspareunia)
- Pelvic organ prolapse
- Constipation or difficulty with bowel movements
- Vaginal pain or discomfort
This treatment can be especially beneficial for individuals who have not found relief from traditional pelvic floor therapies or those who are seeking a complementary approach to other treatments.
The Dry Needling Procedure for Pelvic Floor Treatment
The procedure for dry needling in pelvic floor therapy is highly individualized and typically involves several steps:
Initial Assessment and Evaluation
Before beginning treatment, the physical therapist will thoroughly evaluate the patient’s pelvic floor muscles and overall health. This evaluation may include palpation of the pelvic region to identify areas of tension, pain, or dysfunction.
Selection of Appropriate Needles
The physical therapist will choose thin, sterile needles appropriate for the treatment area. These needles are specifically designed for dry needling and are much thinner than those used for injections or acupuncture.
Insertion of Needles into Trigger Points
Once the appropriate areas are identified, the physical therapist will insert the needles into the trigger points or tight muscles within the pelvic floor. This insertion is typically painless or causes minimal discomfort.
Manipulation of Needles to Elicit a Twitch Response
The therapist will then manipulate the needles to elicit a twitch response, which is a sign that the muscle is releasing tension. This can lead to significant relief of pain and improved muscle function.
Removal of Needles and Post-Treatment Care
After the needles have been in place for a few minutes, they will be removed. The physical therapist may recommend specific stretches or exercises to help maintain the benefits of the dry needling treatment.
Risks and Side Effects
While dry needling is generally considered safe, there are some potential risks and side effects. These may include:
- Mild bruising at the needle insertion site
- Temporary soreness or tenderness
- Lightheadedness or dizziness (rare)
- Slight increase in pain before feeling relief
Does dry needling cause pain? It’s a common question, and while you may feel some mild discomfort during or after treatment, it’s generally temporary. Most people experience relief after a session or two. As with any treatment, it’s important to communicate with your physical therapist about any discomfort to ensure that adjustments can be made.
How to Find a Qualified Professional for Dry Needling
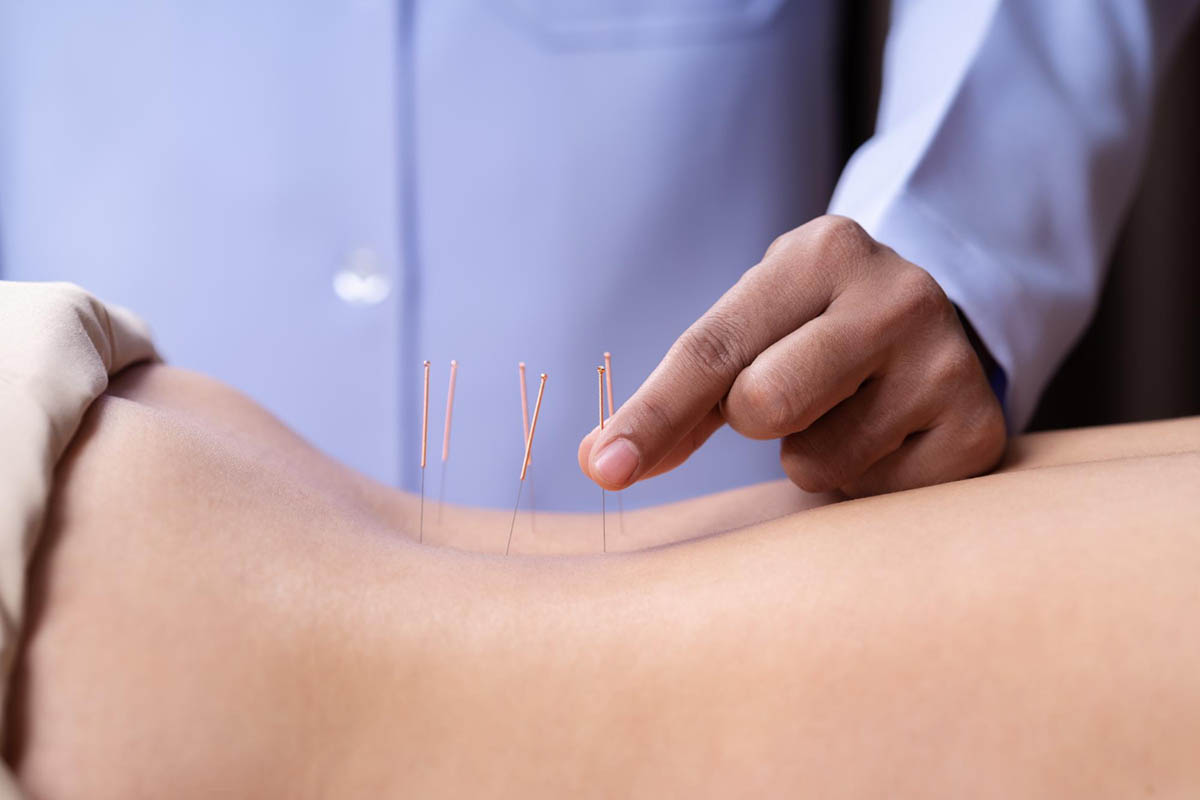
Finding a qualified physical therapist who is trained in dry needling for pelvic floor dysfunction is crucial to ensure the treatment is effective and safe. Look for licensed therapists who have completed additional certification in dry needling techniques. You may search for “pelvic floor dry needling near me” or inquire about the therapist’s experience with dry needling specifically for pelvic issues.
Conclusion
Dry needling is a promising treatment for pelvic floor dysfunction that offers pain relief, improved muscle function, and enhanced quality of life. Whether you’re dealing with chronic pelvic pain, urinary issues, or sexual discomfort, dry needling can provide significant benefits when used as part of a comprehensive pelvic floor therapy plan.
FAQs
What does dry needling do for the pelvic floor?
Dry needling targets tight, painful muscles in the pelvic floor, helping to release tension, improve blood flow, and relieve pain. It can also improve bladder and bowel control and help restore muscle function.
When should you not use dry needling?
Dry needling should not be used if you have certain health conditions, such as active infections, blood clotting disorders, or pregnancy. Always consult with a healthcare professional before beginning treatment.
How many sessions of dry needling are needed?
The number of sessions needed will depend on the severity of the pelvic floor dysfunction and the patient’s response to treatment. One study reported relief of pain and improved mobility after 5–7 sessions of dry needling for chronic pelvic pain. Your physical therapist will recommend the appropriate sessions based on your individual needs.